While pricing transparency is now required by law, the initiative has largely fallen short of its lofty promise to transform the healthcare industry by empowering members and driving down sky-high costs.
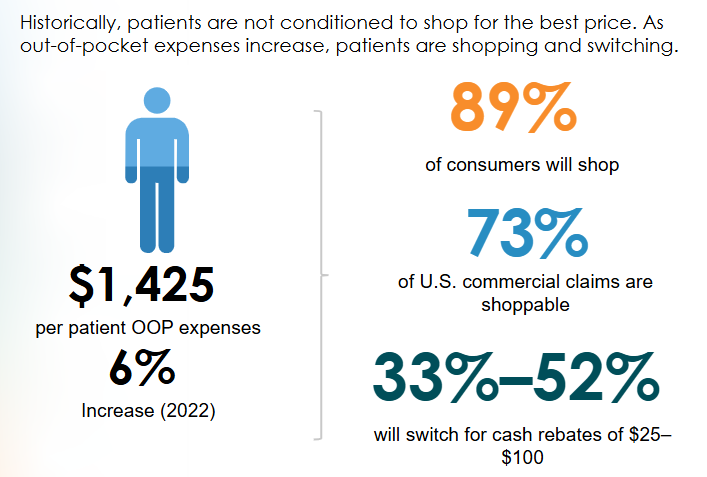
Although 58% of American say they are willing to “shop” for healthcare if pricing information is disclosed prior to services being rendered, changing established customer behavior has proven more difficult than anticipated, in part due to a lack of awareness and understanding about the programs and tools available to them.
This paradox highlights the key challenge with today’s transparency efforts: Simply providing access to information doesn’t guarantee action by members.
To influence healthcare decisions that significantly contain costs and improve quality of care, transparency must always be paired with meaningful financial incentives.
Vālenz Health® recognizes the critical importance that education and engagement play in supporting smarter, better, faster healthcare decisions. That’s why we lead the industry in offering comprehensive strategies that engage early and often to guide members toward lower-cost, higher-value care choices — choices that are rewarded with personalized, meaningful incentives.
Today, we’ll show you just how those strategies work at scale to help optimize the cost, quality, and utilization of healthcare for everyone — and how we can help you do the same with your benefits plan strategy.
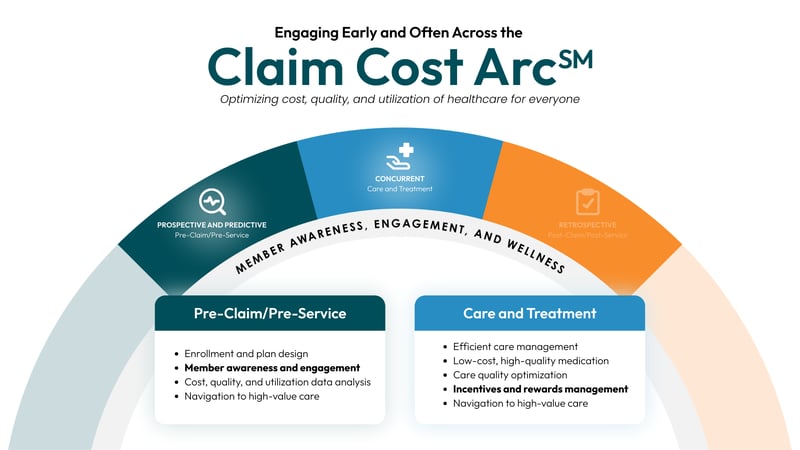
The Limitations of Traditional Price Transparency Tools
As part of a push for more transparent practices in the healthcare industry, the U.S. federal government passed the Transparency in Coverage rules and the No Surprises Act, both of which work together to minimize the risk of unexpected costs to members by requiring accurate estimates for procedures before care is ever delivered.
Unfortunately, many resulting price transparency tools were designed solely to meet these regulatory standards, not necessarily with the member experience in mind. As a result, existing tools are confusing and burdensome to use, with information presented in a complex manner that’s difficult to interpret, delivered after care decisions are already made, or lacking context around quality or outcomes (which is a critical piece of the value-based care model).
That’s if members even use the tools at all. Research consistently shows that less than 10% of patients consistently use price transparency tools to review their care options, revealing a huge opportunity cost for plans and providers alike.
Why Behavior Change Requires Tangible Incentives
Price transparency is often lauded as a powerful way to encourage members toward smarter healthcare choices. The reality is a bit more complicated.
Most plan members make care choices based on a variety of factors, including a sense of habit, urgency to receive care, and referrals from their current providers. Price comparison doesn’t always enter that discussion, especially if members are unaware of the transparency tools available to them.
As a result, those other priorities often win out when members are making healthcare choices — which means today’s plan designers cannot rely solely on the existence of pricing information to significantly influence patient behavior.
That’s where meaningful, well-design incentives strategies step in to fill the gap.
Plan members are more likely to act contrary to their established behavior patterns when there is a clear, immediate benefit to doing so. For example, according to a 2023 McKinsey study, 33–52% of consumers are willing to switch providers or health systems in return for cash updates of $25 to $100 — demonstrating the effectiveness of direct financial rewards in changing patient behavior.
When paired with consistent education and engagement strategies, financial incentives help patients overcome the embedded obstacle of “how things are always done” by giving them a tangible, obvious reason to change their behavior. As a result, by simplifying the decision-making process and providing clear benefits to certain providers over others, incentive strategies can be extremely effective in aligning member behavior with overarching cost-containment plan goals.
Consider the case of a long-term Valenz client that implemented a rewards strategy to boost member usage of the Valenz Bluebook price transparency tool. In the second year of implementation, the program distributed more than 300 rewards to members who used the platform to shop for care — an investment that paid back in dividends for $239,000 in total savings and a 7:1 return on investment.
In short, incentives in the form of financial rewards are the “activation layer” missing from many price transparency initiatives today — the piece of the puzzle that turns insights into action and action into measurable results for both plans and plan members.
Turning Transparency into Action: How Vālenz Health® Incorporates Incentives into Member Engagement
At Valenz, we understand what many leaders in the industry fail to grasp: that information alone does not change consumer behavior.
That’s why we’ve developed a comprehensive member engagement solution suite that engages early and often to influence smarter decision making, guiding members to lower-cost, higher-quality care options that simultaneously reduce spend and support better health outcomes.
Our incentives programming is deployed through two separate solutions: Valenz Variable Copay and Valenz Bluebook Engagement Rewards.
Embedding Financial Rewards at the Point of Decision: Valenz Variable Copay
The most effective way to change member decision-making behavior? Provide them tangible, obvious financial incentives at the moment they make their provider choice.
We make that possible with Variable Copay, a dynamic copay pricing solution that embeds directly into existing networks to identify and highlight high-value providers. By assigning lower copays to those providers proven to deliver better care outcomes at a lower cost, our solution clearly illuminates how much members can save on out-of-pocket costs when they choose the right providers.
Variable Copay uses the power of the Valenz Bluebook price and quality transparency platform to map more than 2,000 common medical procedures to clear, predictable copays, targeting 46% of medical spend for an average estimated 7–12% savings for employers.
We simplify the process of finding high-quality, low-cost care for members by giving clear, easy-to-understand financial signals, highlighted with our “green-yellow-red" ranking system. In doing so, we upend the traditional, fee-for-service-based thinking that “more is better” — a misleading concept in an industry where higher prices are not always asssociated with higher-quality care outcomes.
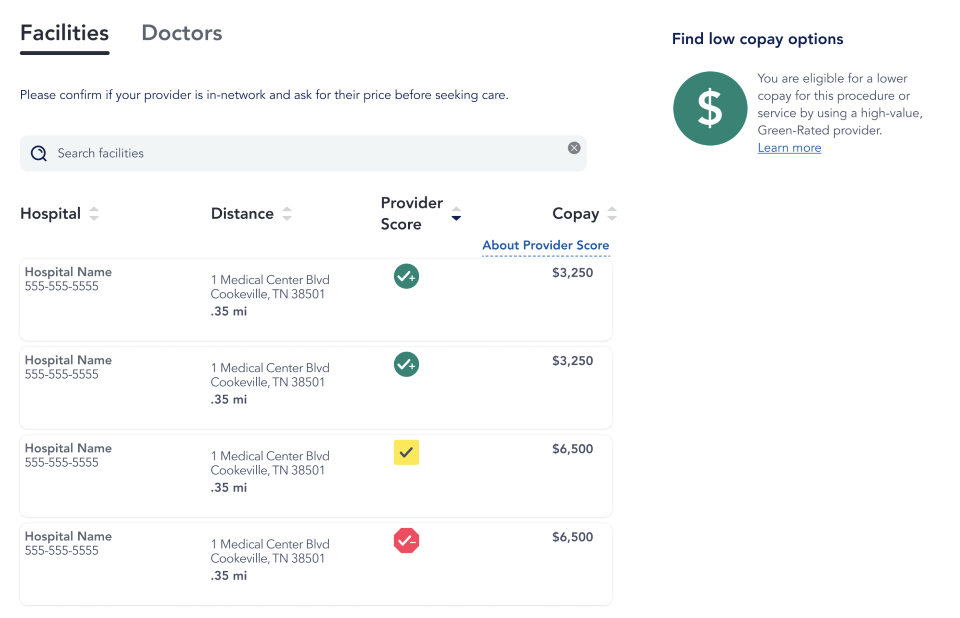 As a result, Variable Copay not only delivers better cost-containment for plans and patients at the moment of decision. It also steers care utilization toward higher-quality providers that reduce unnecessary or overpriced care usage over time — supporting a value-based care model that benefits members, employers, and plan sponsors with a long-term, quality-focused approach toward the healthcare system.
As a result, Variable Copay not only delivers better cost-containment for plans and patients at the moment of decision. It also steers care utilization toward higher-quality providers that reduce unnecessary or overpriced care usage over time — supporting a value-based care model that benefits members, employers, and plan sponsors with a long-term, quality-focused approach toward the healthcare system.
 Changing Decision-Making Culture with Post-Care Incentives: Valenz Bluebook Engagement Rewards
Changing Decision-Making Culture with Post-Care Incentives: Valenz Bluebook Engagement Rewards
Changing consumer behavior is a long-term strategy, one that requires consistent education and reminders for plan members.
Engagement Rewards (a feature of the Valenz Bluebook solution) makes that easy with a strategic, personalized approach to rewards and engagement programming.
By offering additional financial rewards after care is received, Engagement Rewards keeps the Valenz Bluebook tool at the top of mind for members — reiterating the importance of shopping for healthcare after the immediate member care needs are met.
Every time a member uses Valenz Bluebook to shop for and select high-value care, they receive a financial reward (via debit card, HSA or HRA contributions, and/or wellness points) to congratulate them on their informed decision.
At the same time, our team deploys personalized outreach and engagement communications to educate members about their “shoppable” care options, including the potential rewards they can receive when they continue to leverage the Valenz Bluebook platform during their provider search.

By combining optimized outreach campaigns with high-value financial incentives, Engagement Rewards educates and reminds members about the price and quality data available to them, changing member behavior over time and establishing a consumer culture of shopping for care before ever stepping into a provider’s office.
The success of our approach is obvious, as demonstrated by the 2.6x return on investment achieved by one Valenz client in the first year of implementation alone.
%20Case%20Study/chart-movement-of-cases-from-high-cost-to-low-cost.png?width=800&height=408&name=chart-movement-of-cases-from-high-cost-to-low-cost.png) Amplify the Impact of Transparency Tools with Engagement and Rewards Strategies Toda
Amplify the Impact of Transparency Tools with Engagement and Rewards Strategies Toda
Despite the promise of newly implemented price transparency tools, the lack of uptake by members in the last decade proves that information alone is not enough to change member decision making.
To maximize the success of price and quality transparency tools, health plan designers must also invest in comprehensive engagement strategies that use financial incentives to change member behavior and encourage smarter, better care choices.
Those employers that combine industry-leading data transparency with strategic incentive design will be better positioned to control costs and improve care outcomes over the long term — which will remain critical as the industry faces down the challenge of ever-rising healthcare costs.
Thanks to our comprehensive, innovative approach to member engagement, Valenz is uniquely positioned to help self-funded employers and plan sponsors incorporate education and rewards strategies into existing plan designs. Our solutions are designed for ease of implementation, integrating directly with your current provider network to reduce friction and maximize immediate uptake by your covered members from day one.
Learn more about our solutions — or start designing your personalized engagement strategy — by contacting our team today.