If the last decade is any indication, exponentially increasing healthcare costs are here to stay, making strategic, innovative cost containment a non-negotiable for today’s plan payers.
Recent reports put expected medical cost increases for the group market at 8.5% in 2026, with the total health benefit cost per employee anticipated to rise by 6.5%. At the same time, employers who choose not to implement cost-management measures could see up to a 9% increase in costs this year.
For self-funded employers, therefore, the question is no longer whether or by how much costs will rise — but how to manage these financial pressures while still delivering high-quality healthcare coverage for employees.
At Vālenz Health®, we understand self-funded employers’ urgent need for smarter, better, faster healthcare solutions that contain costs without compromising quality of care. That’s why we’ve developed a proactive, integrated approach to reducing expenses before, during, and after care is received — a strategy outlined in our latest white paper, “Navigating Rising Healthcare Costs: A Roadmap for Self-Funded Employers.”
Below, preview some of our recommendations for self-funded employers looking to reduce their health plan expenses in 2026.
For the full roadmap, including actionable ways that Valenz can help you optimize the cost, quality, and utilization of healthcare this year, download our white paper today.
Engaging Early and Often for a Full-Cycle Approach to Cost Containment
Amid rising healthcare costs, self-funded employers are in an elevated position of risk: They directly assume the financial responsibility of high-dollar member claims, which are steadily climbing in both cost and frequency.
At the same time, self-insured employers must maintain comprehensive benefit offerings to attract and retain top talent. Cutting benefits or shifting more cost-sharing to members is not the right solution, especially when healthcare coverage is the top priority for today’s job seekers.
Enter the full-cycle cost-containment strategy from Valenz, illustrated by our Claim Cost Arc℠.

The Valenz Claim Cost Arc simplifies healthcare by splitting the care journey into three distinct phases: prospective, concurrent, and retrospective. Health literacy and data-driven decision making are integrated into each stage (from pre-service to treatment to post-service) to illustrate the value of engaging early and often to capture and identify cost-savings opportunities.
Using this approach, self-funded employers can significantly reduce costs, improve care quality, and elevate the entire healthcare experience — supporting their employees in living strong, vigorous, and healthy lives without an unsustainably high price tag.
Read more about this concept in action in our case study, where we share how the Valenz full-cycle solution saved one group $4.3 million in its first year of implementation.
Addressing Rising Healthcare Costs with Innovative Cost-Containment Strategies
While overall inflation trends play a significant role in rising healthcare costs, other factors are more variable and nuanced, meaning a single solution targeted at one stage of the care journey is unlikely to deliver significant savings.
It’s critical, then, that self-funded employers align with strategic partners like Valenz to implement integrated solutions that work across the Claims Cost Arc to mitigate financial burdens while ensuring members can still access and receive high-value healthcare.
To kickstart your cost-containment efforts, we’ve recommended a few of our highest-impact strategies, which capture cost savings before, during, and after care is received.
Use them as a starting point for designing your benefits plan strategy — and, when you’re ready to make smarter, better, faster healthcare a reality for your self-funded plan, know we will be standing by to help.
Empower Members with Transparent Quality and Cost Data
Stronger cost containment starts with smarter member care choices. Research has shown that well-informed patients often choose less aggressive and costly therapies, with improvements to healthcare literacy associated with a decrease in overall costs.
The key is in providing members with the tools they need to make those high-value, low-cost care choices.
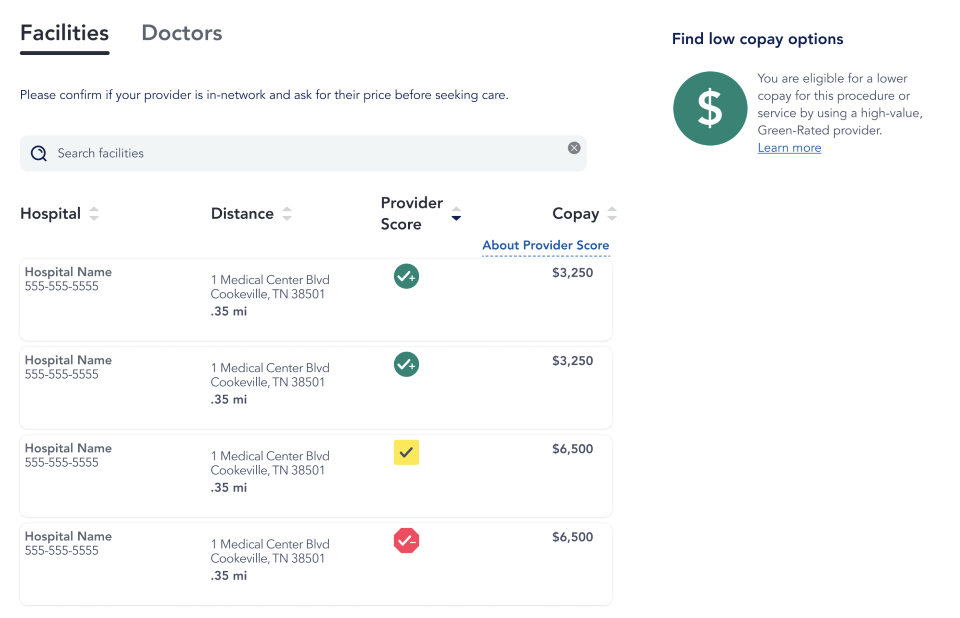
Self-funded employers looking to reduce costs should prioritize comprehensive quality and pricing data tools like Valenz Bluebook. These tools help members find in-network providers who perform common shoppable procedures, allowing them to sort by estimated out-of-pocket costs, care quality rankings, travel distance, and other important factors.
Original analysis estimated that price transparency tools would save as much as $80 billion in costs between 2023 and 2025. With Valenz Bluebook, the cost containment is just as significant; every time a member uses the tool, employers can expect an average savings of $1,500.
With data for more than 4,000 facilities and 500,000 providers, plus quality rankings for more than 200 procedures, Valenz Bluebook provides the most comprehensive transparency tool in the market. Our color-coded, “red-yellow-green" ranking system makes it easy for members to find high-quality care at a Fair Price™, supporting smarter decision making that saves both patient and payer money before care is ever accessed.

To further incentivize the choice of high-value, low-cost care, self-funded employers can employ rewards campaigns that offer financial benefits to employees. For example, with the Engagement Rewards feature, employees are issued rewards via debit card, HSA/HRA contributions, and/or wellness points when they shop and receive care using Valenz Bluebook.
With Valenz Variable Copay, the financial incentives are even more immediate; members can see the direct correlation between lower copays and higher-quality care, guiding choices that deliver higher savings for both them and the overall plan.
 Learn more about these solutions and unlock your savings potential by contacting us today.
Learn more about these solutions and unlock your savings potential by contacting us today.
Design Networks for High-Value Care
To direct members to high-value, low-cost care options that are covered under their plan, self-funded employers must also prioritize network designs that offer those options in the first place.
As a contrast to traditional networks, expanded options such as contracted, high-performance narrow networks or non-contracted, reimbursement-based networks can guide members to high-value providers and facilities with optimal outcomes — and minimal costs.
Research shows that when members use providers that prioritize care outcomes as part of a value-based healthcare system, the number of readmissions and complications (as well as associated expenses) is significantly reduced when compared to non-value-based care.
Because they are not tied into the PPO network often required by a fully funded plan, self-funded employers have the advantage of personally designing their networks to maximize the savings of a value-based plan.
With our High-Performance Networks, a feature of In-Network Repricing, Valenz can help make that happen.
Using our extensive dataset of quality and outcomes metrics, we rigorously analyze facilities and providers to meet our high standards, consolidating top performers into a highly efficient collective that meets members’ care needs and an employer’s plan requirements. As a result, we remove the risk of balance billing and improve care utilization, delivering an average 20–40% improvement in savings compared to traditional BUCAH plans.
Build a high-performance network that reduces costs while protecting care quality by contacting our team members today.
Protect Your Plan with Stop Loss Insurance
Even with cost-containment strategies in place, unexpected high-cost claims can (and often do) still happen, putting a serious burden on self-funded employers who are responsible for those costs.
Stop loss insurance proactively works to protect employers from that risk by providing a much-needed financial safety net, setting a threshold beyond which they are reimbursed for unexpected claim costs.

Like other cost-containment efforts, stop loss policies can be underwritten to meet the specific needs of members, the plan payer’s budget, and other factors. More importantly, stop loss underwriters like those at Valenz can take cost-containment strategies into account when designing a policy, reducing plan premiums when employers demonstrate a commitment to high-value, low-cost care.
With 88% of employers experiencing a stop loss claim each year, today's self-funded employers cannot overlook the importance of this strategy as a response to rising healthcare costs. Fortunately, when employers partner with the stop loss leaders at Valenz, they can secure this financial protection and relevant cost-containment solutions from a single provider, with average premium savings up to 50%.
 Request a stop loss quote for your self-funded insurance plan by contacting our team today.
Request a stop loss quote for your self-funded insurance plan by contacting our team today.
Eliminate and Resolve Billing and Payment Errors
While payment integrity solutions are commonly deployed to minimize claims costs after care is delivered, few self-funded employers also invest in solutions that engage before and during the care journey. Like member engagement and plan design, payment integrity is a full-cycle strategy, which is why it anchors our roadmap for employers looking to contain rising healthcare costs.
From designing high-value networks of providers with histories of clean claims to repricing claims based on market-sensitive, defensible rates, full-cycle payment integrity solutions engage early and often to capture savings opportunities before payments are made, delivering higher savings on average than more reactive approaches.
Software that incorporates automation allows for faster preapproval and claims review, freeing up the time for clinical billing experts to manually review those claims brought to their attention based on pattern recognition and extensive data analysis. And, with 54% of healthcare providers reporting that claims errors are actively increasing, the need for innovative, comprehensive payment integrity solutions will only grow.
To avoid the outsized financial risk that comes with self-funding, today’s employers must invest in these full-cycle solutions to ensure appropriate, accurate charges and defensible payments. Valenz offers these services in one integrated, customizable platform, supporting the interchange of valuable provider and billing data across the Claims Cost Arc for smarter, better, faster cost containment.
Unlock your savings potential by contacting our payment integrity team today.
Take an Innovative Step toward Smarter, Better, Faster Healthcare Today
While consistently increasing healthcare costs are a challenge for self-funded employers, they also present a new opportunity: the chance to innovate with alternative plan designs that prioritize cost containment throughout the care journey.
Here at Valenz, we’re leading that charge by transforming outdated cost-sharing models into a predictable variable copay structure that steers members toward high-value, low-cost care and improves their overall experience.
By incentivizing patients to make smarter care choices, ValenzONE minimizes both out-of-pocket costs for members and overall plan costs for self-funded employers, delivering an average of 7–12% savings for payers who implement the Variable Copay solution. 
Through the integration of predictable copays, proactive navigation, and clear insight into cost and quality, ValenzONE supports high-value decision making throughout the member journey and Claim Cost Arc — supporting the optimization of high-value healthcare for all involved in the journey.
Learn more about the transformative power of ValenzONE by contacting one of our team members below.
In the meantime, dive deeper into our full suite of comprehensive cost-containment solutions — and how they work across the Claim Cost Arc to reduce expenses for self-funded employers — by downloading our latest white paper today.

